Why Teens Need Quality Sleep
Teenagers require 8‑10 hours of sleep each night, with most experts citing about nine hours for optimal brain development and emotional regulation. When adolescents consistently miss this amount, they suffer impaired concentration, lower academic grades, heightened anxiety or depression, and increased impulsivity that can lead to risky driving or substance use. Chronic sleep debt also disrupts hormone balance, raising obesity and diabetes risk. Families play a crucial role: setting consistent bedtime rules, limiting evening screen exposure, and creating a cool, dark bedroom support healthy habits. Pediatricians should screen for insomnia, mood disorders, and sleep‑related health issues, referring persistent problems to specialists to protect a teen’s long‑term wellbeing and future success.
The Scope and Roots of the Problem
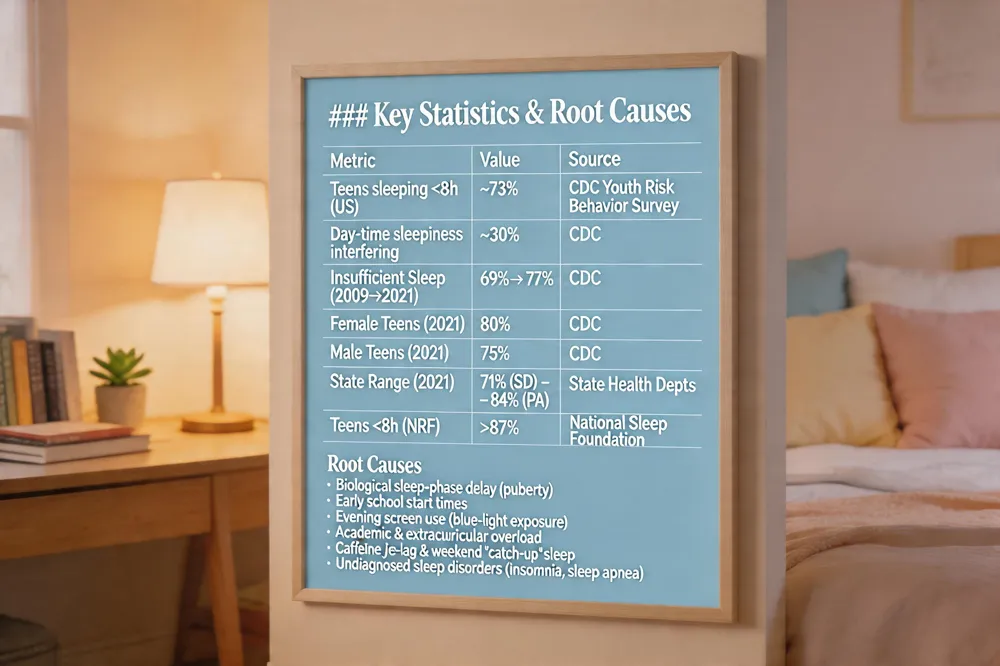
Key Statistics & Root Causes
| Metric | Value | Source |
|---|---|---|
| Teens sleeping <8 h (US) | ~73 % | CDC Youth Risk Behavior Survey |
| Day‑time sleepiness interfering with activities | ~30 % | CDC |
| Insufficient sleep prevalence (2009→2021) | 69 % → 77 % | CDC |
| Female teens reporting short sleep (2021) | 80 % | CDC |
| Male teens reporting short sleep (2021) | 75 % | CDC |
| State range (2021) | 71 % (SD) – 84 % (PA) | State health departments |
| Teens getting <8 h (NRF poll) | >87 % | National Sleep Foundation |
Root Causes
- Biological sleep‑phase delay (puberty)
- Early school start times
- Evening screen use (blue‑light exposure)
- Academic & extracurricular overload
- Caffeine consumption
- Social jet‑lag & weekend “catch‑up” sleep
- Undiagnosed sleep disorders (insomnia, sleep apnea)
 Sleep deprivation in teens statistics
Sleep deprivation in teens statistics
In the United States, roughly 73 % of high‑school students report getting fewer than the recommended 8–10 hours of sleep on school nights, and about 30 % experience daytime sleepiness that interferes with daily activities. The CDC’s Youth Risk Behavior Survey shows that the prevalence of insufficient sleep has risen from 69 % in 2009 to 77 % in 2021, with 80 % of female teens and 75 % of male teens reporting short sleep duration in 2021. State‑level data reveal a range from 71 % in South Dakota to 84 % in Pennsylvania in 2021. Earlier National Sleep Foundation polling indicated that more than 87 % of U.S. teens get far less than the recommended 8–10 hours. Together, these figures underscore a national epidemic of teen sleep deprivation with significant health and safety implications.
Causes of teenage sleep deprivation
Teenage sleep loss arises from a blend of biological, academic, and lifestyle factors. A natural sleep‑phase delay pushes teens’ internal clocks later, yet early school start times force awakening before they are fully rested. Electronic device use before bedtime—texting, social media, video games—exposes teens to blue light that suppresses melatonin and delays sleep onset. Academic pressures, extracurricular activities, part‑time jobs, and caffeine consumption further compress bedtime. Social jet‑lag from weekend “catch‑up” sleep and undiagnosed sleep disorders such as insomnia or sleep apnea can exacerbate chronic sleep debt, creating a cycle that harms mood, cognition, and safety.
How Lack of Sleep Affects the Brain and Body
Neuro‑cognitive & Physiological Impacts
| Effect | Domain | Impact |
|---|---|---|
| Reduced prefrontal cortex activity | Executive function | Poor decision‑making, planning, impulse control |
| Impaired hippocampal consolidation | Memory | Lower learning retention, difficulty recalling information |
| Disrupted emotional regulation circuits | Mood | ↑ irritability, anxiety, depression, suicidal thoughts |
| Decreased REM & deep‑sleep | Synaptic pruning & connectivity | Slower cognitive development, higher risky‑behavior risk |
| Metabolic dysregulation | Metabolism | ↑ obesity, type 2 diabetes, cardiovascular risk |
| Immune suppression | Immune system | Greater susceptibility to illness |
| Slower reflexes & impaired judgment | Physical performance | ↑ sports injuries, falls, drowsy‑driving crashes |
 Teenagers are caught in a perfect storm of biology and schedule: a puberty‑driven sleep‑phase delay pushes natural bedtime two hours later, yet early school start times (often before 8 a.m.) force them awake before they are ready. More than 87 % of U.S. high‑school students therefore get far less than the recommended 8‑10 hours of sleep, creating chronic sleep debt that harms both mind and body.
Teenagers are caught in a perfect storm of biology and schedule: a puberty‑driven sleep‑phase delay pushes natural bedtime two hours later, yet early school start times (often before 8 a.m.) force them awake before they are ready. More than 87 % of U.S. high‑school students therefore get far less than the recommended 8‑10 hours of sleep, creating chronic sleep debt that harms both mind and body.
Effects of sleep deprivation on teenage brain
Sleep deprivation markedly lowers activity in the prefrontal cortex, weakening executive functions such as decision‑making, planning, and impulse control. It also disrupts the hippocampus’s role in memory consolidation, leading to poorer learning, reduced retention, and difficulty recalling information. Chronic lack of sleep interferes with emotional regulation circuits, heightening irritability, anxiety, depression, and suicidal thoughts in teenagers. Reduced REM and deep‑sleep phases impair synaptic pruning and brain‑wide connectivity, slowing overall cognitive development. These neural deficits increase the risk of risky behavior, accidents, and long‑term mental‑health problems.
Long‑term effects of sleep deprivation in teens
Persistently short sleep impairs memory, attention, and academic achievement, making it harder to keep up in school. It disrupts emotional regulation, raising the odds of anxiety, depression, and suicidal thoughts. Metabolic changes promote obesity, type 2 diabetes, and cardiovascular risk, while a weakened immune system leaves teens more vulnerable to illness. Drowsy‑driving incidents surge, with crash rates climbing in districts that start school later, underscoring the safety hazard of inadequate rest.
Sleep‑related injury and accident risk
Beyond motor‑vehicle crashes, sleep‑deprived teens experience slower reflexes, clumsiness, and impaired judgment, increasing the likelihood of sports injuries, falls, and other accidents. Early identification of chronic sleep loss and prompt medical evaluation—especially when symptoms mimic ADHD or insomnia—are essential to protect teen health and prevent lasting harm.
What Teens Experience Day‑to‑Day
Typical Day‑to‑Day Symptoms
| Symptom | Typical Frequency | Consequence |
|---|---|---|
| Daytime drowsiness | Daily for most teens | Reduced alertness, micro‑napses |
| Mood swings & irritability | Several times/week | Strained relationships, conflict |
| Trouble concentrating | Daily in class | Lower grades, academic struggles |
| Slower reaction time | Often during sports/ driving | Higher injury & crash risk |
| Weight gain/obesity | Gradual over months | Metabolic health concerns |
| Anxiety & depressive thoughts | Intermittent to frequent | Mental‑health risk, possible suicidal ideation |
 Teenage sleep patterns are driven by a biological sleep‑phase delay that pushes bedtime two hours later, while the recommended 9–9½ hours of sleep is rarely achieved. Most U.S. high‑schoolers get only 6–7 hours because school starts before 8 a.m., homework, sports and and screen time encroach on the evening. This chronic sleep debt shows up as daytime drowsiness, irritability, and trouble concentrating, which hurt grades and increase drowsy‑driving crashes.
Teenage sleep patterns are driven by a biological sleep‑phase delay that pushes bedtime two hours later, while the recommended 9–9½ hours of sleep is rarely achieved. Most U.S. high‑schoolers get only 6–7 hours because school starts before 8 a.m., homework, sports and and screen time encroach on the evening. This chronic sleep debt shows up as daytime drowsiness, irritability, and trouble concentrating, which hurt grades and increase drowsy‑driving crashes.
For a 15‑year‑old, insufficient sleep means foggy cognition, slower reaction times, and poorer athletic performance. Mood swings, anxiety, and a heightened risk of depression become common, and the hormonal imbalance can promote weight gain and obesity. Weekend “catch‑up” sleep only partially restores the deficit; a consistent nightly routine is essential.
Key strategies: set a regular bedtime and wake time (even on weekends), limit electronic screens at least an hour before bed, keep the bedroom cool, dark, and quiet, and encourage a brief early‑afternoon nap if needed. If your teen still struggles with falling asleep, daytime sleepiness, or snoring, consult your pediatrician for a thorough evaluation.
Practical Strategies and When to Seek Professional Help
Actionable Strategies & Referral Triggers
| Strategy | Description | When to Seek Professional Help |
|---|---|---|
| Consistent bedtime & wake‑time (including weekends) | Sets circadian rhythm | Persistent insomnia >4 weeks despite routine |
| Limit screens ≥1 h before bed | Reduces blue‑light melatonin suppression | Ongoing difficulty falling asleep |
| Cool, dark, quiet bedroom | Optimizes sleep environment | Continuous fragmented sleep or snoring |
| Daily physical activity (avoid vigorous late‑evening) | Improves sleep drive | Excessive daytime sleepiness despite activity |
| Reduce caffeine after lunch | Prevents stimulant effect | Sleep onset latency >30 min daily |
| Structured homework / extracurricular schedule | Prevents overload | Academic performance dropping due to fatigue |
| Screen‑down wind‑down routine (reading, breathing) | Calms nervous system | Mood/energy swings linked to poor sleep |
| Referral | If any of the following appear: loud snoring, gasping pauses, chronic pain, sudden mood/energy/appetite changes, or symptoms suggest sleep apnea/insomnia → pediatrician or sleep specialist | – |
 WhyHow to solve sleep deprivation in teens? Teens need 8‑10 hours of sleep, a so biologically‑driven sleep‑phase delay pushes bedtime later. Establish a regular bedtime and wake‑time, limit screen exposure at least one hour before bed, and keep the bedroom cool, dark, and quiet. Encourage daily physical activity but avoid vigorous exercise close to bedtime, and cut back on caffeine or sugary drinks in the late afternoon. Help teens manage schoolwork and extracurriculars with a realistic schedule and a calming wind‑down routine (deep‑breathing, reading, gentle yoga). If these hygiene steps don’t improve sleep, a pediatric evaluation is warranted to rule out medical or mental‑health issues.
WhyHow to solve sleep deprivation in teens? Teens need 8‑10 hours of sleep, a so biologically‑driven sleep‑phase delay pushes bedtime later. Establish a regular bedtime and wake‑time, limit screen exposure at least one hour before bed, and keep the bedroom cool, dark, and quiet. Encourage daily physical activity but avoid vigorous exercise close to bedtime, and cut back on caffeine or sugary drinks in the late afternoon. Help teens manage schoolwork and extracurriculars with a realistic schedule and a calming wind‑down routine (deep‑breathing, reading, gentle yoga). If these hygiene steps don’t improve sleep, a pediatric evaluation is warranted to rule out medical or mental‑health issues.
When to go to the doctor for sleep problems? Seek professional help if difficulty falling or staying asleep persists beyond four weeks, interferes with school or sports, or is accompanied by loud snoring, gasping pauses, persistent pain, or sudden changes in mood, energy, or appetite. These signs may indicate sleep apnea, insomnia, or underlying health concerns that need medical assessment.
How much sleep should a 16‑year‑old get? The recommended range is 8‑10 hours, with the sweet spot around 9 hours ± ½ hour. Consistently meeting this target supports learning, mood regulation, athletic performance, and reduces risks of obesity, depression, and accidents. Parents can reinforce healthy habits by maintaining consistent bedtime rules, limiting evening caffeine and screens, and ensuring exposure to natural daylight during the day.
Supplements, Rules, and Night‑Time Tips
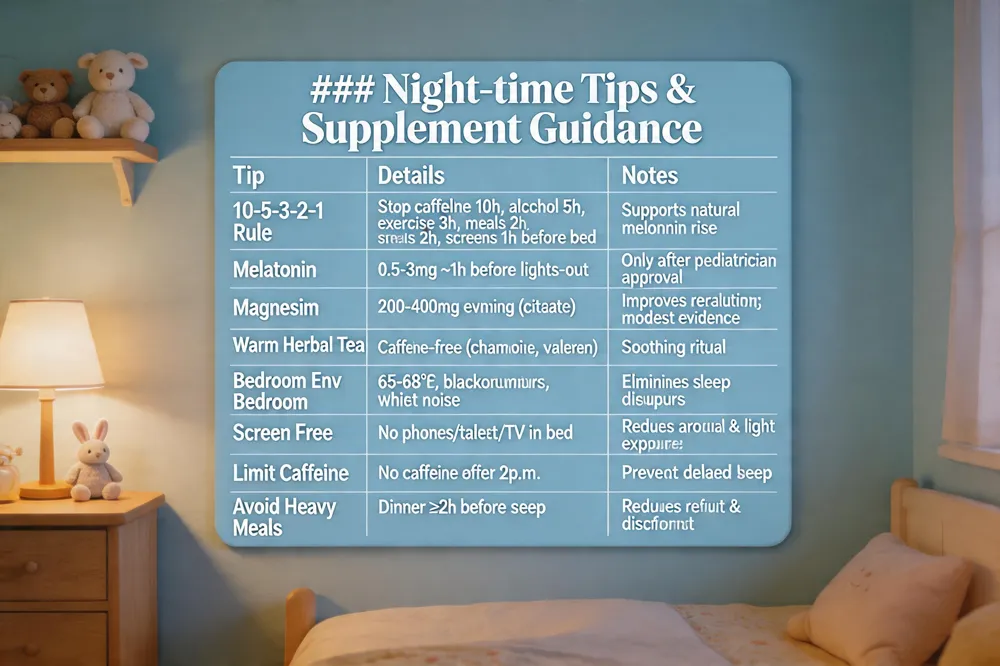
Night‑time Tips & Supplement Guidance
| Tip | Details | Notes |
|---|---|---|
| 10‑5‑3‑2‑1 Rule | Stop caffeine 10 h, alcohol 5 h, vigorous exercise 3 h, heavy meals 2 h, screens 1 h before bedtime | Supports natural melatonin rise |
| Melatonin | Low dose 0.5‑3 mg taken ~1 h before lights‑out | Use only after pediatrician approval |
| Magnesium | 200‑400 mg in the evening (e.g., magnesium citrate) | May improve relaxation; evidence modest |
| Warm herbal tea | Caffeine‑free (chamomile, valerian) | Helpful soothing ritual |
| Bedroom environment | Cool (≈65‑68 °F), blackout curtains, white‑noise if needed | Eliminates external sleepors |
| Screen‑free bedroom | No phones, tablets, TVs in bed | Reduces mental arousal & light exposure |
| Limit caffeine | No caffeinated drinks after 2 p.m. | Prevents delayed sleep onset |
| Avoid heavy meals | Finish dinner ≥2 h before sleep | Reduces reflux & discomfort |
 What to give a 14‑year‑old to sleep? Start with solid sleep hygiene: a cool, dark, quiet bedroom; screen‑free bedroom at least one hour before bed; and the bed reserved for sleep only. If a supplement is needed, a low‑dose melatonin (1–3 mg) taken an hour before lights‑out can help reset the teen’s internal clock, but always discuss it with a pediatrician first. Over‑the‑counter antihistamines (e.g., diphenhydramine) are not recommended for regular teen use, and prescription sleep drugs should be reserved for diagnosed disorders under specialist care. Encourage daytime activity, limit caffeine after lunch, and keep evening meals light.
What to give a 14‑year‑old to sleep? Start with solid sleep hygiene: a cool, dark, quiet bedroom; screen‑free bedroom at least one hour before bed; and the bed reserved for sleep only. If a supplement is needed, a low‑dose melatonin (1–3 mg) taken an hour before lights‑out can help reset the teen’s internal clock, but always discuss it with a pediatrician first. Over‑the‑counter antihistamines (e.g., diphenhydramine) are not recommended for regular teen use, and prescription sleep drugs should be reserved for diagnosed disorders under specialist care. Encourage daytime activity, limit caffeine after lunch, and keep evening meals light.
What can I give my teenager to help with sleep? Prioritize consistent bedtime, a screen‑free bedroom, and caffeine limits. A modest melatonin dose (0.5‑3 mg) before sleep may aid circadian alignment after pediatric approval. Some families find magnesium (200‑400 mg) or a warm caffeine‑free herbal tea (like chamomile) soothing, though evidence is modest. Prescription meds are only for clinically identified sleep disorders and must be prescribed.
What is the 10‑5‑3‑2‑1 rule for sleep? This simple timeline guides evening habits: stop caffeine 10 hours before bedtime, avoid alcohol 5 hours before, finish vigorous exercise 3 hours before, finish heavy meals 2 hours before, and turn off all screens 1 hour before sleep. Following these steps supports natural melatonin rise and better rest.
Key Takeaways for Parents, Teens, and Providers
Teen sleep loss is linked to poor grades, mood swings, anxiety, depression, impulsive risk‑taking, and drowsy‑driving crashes. Warning signs include daytime sleepiness, irritability, difficulty concentrating, frequent naps, and late‑night screen use. To protect health, families should set a consistent bedtime between 8‑10 p.m., keep the bedroom cool, dark, and quiet, turn off electronic devices at least one hour before sleep, limit caffeine after mid‑afternoon, and encourage daily physical activity. A calming wind‑down routine—reading, gentle stretching, or breathing exercises—helps signal sleep. If a teen shows persistent fatigue, mood changes, frequent awakenings, or suspect insomnia, parents should consult a pediatrician for evaluation and possible treatment and develop a sleep plan for long‑term health.
