Welcome to Core Pediatric Care
This article explains why regular medical attention is vital for children and teenagers and how Kids & Teens Primary Healthcare makes that care accessible and supportive for families. The purpose is to highlight the role of well‑child visits, timely immunizations, growth screenings, and mental‑health checks in preventing illness and promoting healthy development. Kids & Teens Primary Healthcare provides family‑centered services from birth through age 21, offering comprehensive well‑child exams, nutrition counseling, chronic‑condition management, and confidential teen health discussions. Their team uses evidence‑based guidelines, offers flexible scheduling and telehealth options, and partners with parents to create a continuous medical home that safeguards each child’s short‑ and long‑term well‑being.
What Pediatric Care Is and Who Provides It
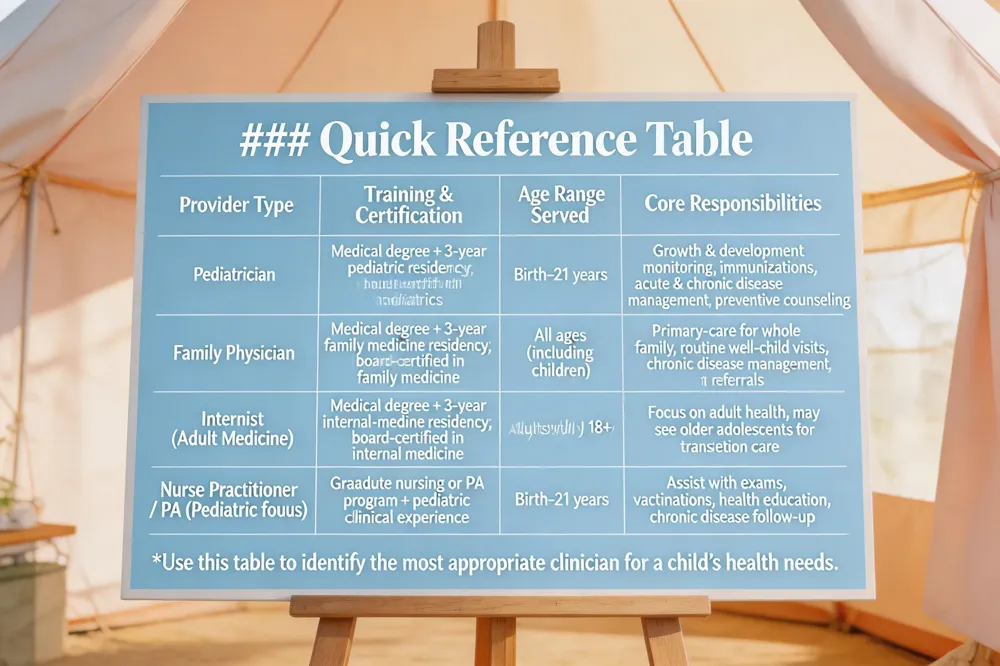 Pediatric care is the specialized medical care for infants, children, adolescents, and young adults up to age 21. It focuses on the physical, emotional, and developmental health of growing patients through preventive services—such as well‑child check‑ups, immunizations, vision and hearing screenings—and the diagnosis and treatment of acute illnesses and chronic conditions like asthma, obesity, and mental‑health concerns. A pediatrician is the doctor who serves as the primary‑care provider for this age group; trained in a three‑year residency after medical school, they understand normal growth curves, developmental milestones, and age‑appropriate nutrition, safety, and behavioral guidance. While pediatricians specialize exclusively in child health, primary‑care physicians—family doctors and some internists—also see children. Family physicians provide care for patients of all ages, making them a convenient option for whole‑family health, whereas internal‑medicine doctors typically focus on adults. Basic knowledge of pediatrics includes growth and developmental surveillance, preventive immunizations (e.g., hepatitis B, DTaP, MMR, annual flu), nutrition counseling, safety measures (car seats, safe sleep), and the ability to coordinate care with specialists when needed.
Well‑Child Visit Schedule and Checklist
 Well‑child visits by age Newborns should be seen at 3–5 days, 1 month, 2 months, 4 months, 6 months, 9 months, and 12 months. After the first year, visits occur at 15 months, 18 months, 2 years (24 months) and 2½ years (30 months). From age 3 through age 10 a well‑child exam is performed yearly, focusing on growth, development, immunizations and safety counseling. Ages 11‑12 continue annual visits that add vision, hearing and mental‑health screening, while teens (13‑18) have yearly exams that include nutrition, sexual‑health education and risk‑behavior counseling. Young adults up to age 21 may schedule a final transition visit to review health maintenance, vaccinations and any ongoing concerns.
Well‑child visit checklist for providers A provider should first review the child’s growth parameters—weight, height, head circumference, and BMI—plotting them on age‑appropriate CDC/AP growth charts and noting any percentile shifts. Next, assess developmental milestones and conduct a comprehensive head‑to‑toe physical exam, including heart, lung, abdominal, musculoskeletal, skin, and sensory (vision and hearing) screenings as indicated by age. Update the immunization record and administer any pending vaccines, while also reviewing newborn screening results and other age‑specific labs such as anemia or lead testing. Provide anticipatory guidance covering nutrition, sleep, physical activity, screen time, safety (home, car, water), and discuss mental‑health red flags, including anxiety, depression, and behavioral concerns. Finally, address parental questions, reinforce preventive counseling, and schedule the next well‑child visit according to the Bright Futures periodicity schedule.
Healthy Habits for Kids and Teens
 Guiding children and adolescents toward lifelong well‑being starts with six core habits.
Nutrition – Offer a colorful variety of fruits, vegetables, whole grains, lean proteins and low‑fat dairy each day, and encourage water instead of sugary drinks.
Physical activity – Aim for at least 60 minutes of moderate‑to‑vigorous movement daily—playing outdoors, biking, sports, dance or age‑building exercises.
Sleep hygiene – Children need 9‑11 hours, teens 8‑10 hours of restful sleep; keep a consistent bedtime routine and a screen‑free wind‑down period.
Stress management – Teach mindfulness, journaling or talking with trusted adults; limit risky behaviors such as vaping, tobacco and excessive alcohol.
Screen time – Keep recreational screen use under two hours for kids and under one hour for school‑age children, replacing extra minutes with active play or reading.
Student health tips – Pack balanced lunches, drink water, practice good posture, take short movement breaks every 20‑30 minutes, and prioritize restorative sleep.
Answering common questions:
- 8 healthy habits for kids – Eat a colorful diet, stay active 60 min, limit screen time, get 9‑11 hrs sleep, brush teeth twice daily, wash hands, schedule well‑child visits, model healthy choices, and maintain a smoke‑free home.
- Healthy habits for teens – Prioritize 8‑10 hrs sleep, balanced diet, 60 min daily activity, good hygiene, stress‑management techniques, and avoid risky substances.
- 5 student health tips – Balanced lunch, hydrate with water, limit screens, practice ergonomics, and ensure consistent restorative sleep.
Preventive Health: Immunizations, Safety, and Developmental Screening
 A solid preventive‑care plan starts with the AAP‑CDC immunization schedule: vaccines such as hepatitis B, DTaP, Hib, IPV, PCV13, rotavirus, MMR, varicella, and annual flu shots protect children from serious disease from birth through age 21. Safety measures—rear‑facing car seats, helmets, smoke detectors, and child‑proofed homes—greatly reduce preventable injuries. At each well‑child visit, pediatricians use tools like the Ages and Stages Questionnaire to screen developmental milestones and refer early for speech, motor, or cognitive delays. Mental‑health screening for anxiety, depression, and behavioral issues begins at age 5 and continues annually, ensuring early support. Finally, dental care should start with the first tooth (brush twice daily with fluoride toothpaste) and vision screenings at preschool age help catch problems that could affect learning.
Family Resources and Access to Care
 Navigating pediatric health becomes easier when families know the tools at their fingertips. Insurance options such as Medicaid and the Children’s Health Insurance Program (CHIP) provide low‑cost or free coverage for most U.S. children, and many pediatric offices have staff who help with enrollment and billing. Patient portals and telehealth let parents view visit notes, request refills, and video‑chat with a pediatrician without leaving home, reducing missed appointments and travel time. After‑hours support—often a 24/7 on‑call line or urgent‑care triage—ensures that urgent concerns are addressed promptly, even when the clinic is closed. Community resources like local health departments, school health programs, and nonprofit parenting workshops offer nutrition classes, immunization clinics, and safety education that complement office‑based care.
What are the core parenting principles? Core parenting principles combine five universal strategies—attention and empathy, predictable daily routines, consistent sequencing within routines, clear household rules, and coaching skills—with the four S’s of attachment (Seen, Soothed, Safe, Secure). Together they promote a nurturing, stable environment that supports children’s emotional and physical development.
Putting It All Together
Key Takeaways: Visits let pediatricians monitor growth, milestones, immunizations and signs of asthma or obesity. Recommended vaccines protect against disease, and breastfeeding for six months followed by a diet with fruits, vegetables, whole grains and protein supports health. Activity, sleep, screen time and safety measures such as car‑seat use and safe sleep are essential.
Next Steps for Parents: Book the next visit per Bright Futures, update immunization records, and complete an Ages and Stages screen. Set routines with meals, bedtime and activity, and verify car‑seat safety. Keep in touch with your pediatrician and discuss mental‑health screening and insurance options.
