Why Spring Allergies Matter
Spring allergies can sap a child’s focus, leading to missed schoolwork and lower grades, while persistent sneezing, congestion, and itchy eyes strain the airway and may trigger asthma or sinus infections. Prompt pediatric evaluation ensures effective treatment and protects health.
Common Childhood Allergens and Symptoms
Allergens vs. Typical Symptoms
| Allergen | Common Symptoms |
|---|---|
| Pollen (tree, grass, weed) | Sneezing, itchy eyes, stuffy nose, “allergy‑shiners” |
| Dust‑mites | Nasal congestion, cough, asthma flare |
| Pet dander | Sneezing, wheezing, itchy eyes |
| Food (milk, egg, peanut, tree nuts, soy, wheat, fish, shellfish, sesame) | Hives, swelling, vomiting, anaphylaxis (severe) |
| Mold | Nasal congestion, cough, asthma symptoms |
| Insect stings | Local swelling, hives, possible anaphylaxis |
 Seasonal allergens—tree, grass, weed pollens, dust‑mites, mold, pet dander—trigger rhinitis in children. Keep windows closed, use AC on recirculate, and shower after outdoor play. Food allergens—milk, eggs, peanuts, tree nuts, soy, wheat, fish, shellfish, and sesame—cause most reactions; milk, eggs and peanuts are frequent, while peanuts, tree nuts, fish and shellfish often cause severe anaphylaxis.
Seasonal allergens—tree, grass, weed pollens, dust‑mites, mold, pet dander—trigger rhinitis in children. Keep windows closed, use AC on recirculate, and shower after outdoor play. Food allergens—milk, eggs, peanuts, tree nuts, soy, wheat, fish, shellfish, and sesame—cause most reactions; milk, eggs and peanuts are frequent, while peanuts, tree nuts, fish and shellfish often cause severe anaphylaxis.
Common allergies Pollen, dust‑mites, pet dander and foods such as milk, eggs, peanuts, tree nuts, soy, wheat, fish, shellfish, and sesame cause sneezing, itchy eyes, asthma, hives, or reactions to insect stings. Allergist consultation helps protect daily life.
Seasonal symptoms Typical signs include a stuffy nose, sneezing, itchy eyes, cough, and dark circles under the eyes (“allergy‑shiners”); some children also develop hives or wheezing during peak pollen periods.
Common food allergies Milk, eggs, peanuts, tree nuts, soy, wheat, fish, shellfish, and sesame cause the majority of child food allergies; milk, eggs and peanuts are frequent, while peanuts, tree nuts, fish and shellfish often lead to severe reactions. 8 % of children under five are affected. Recognizing these triggers helps families keep epinephrine autoinjectors handy.
Environmental Controls to Reduce Pollen Exposure
Quick‑Reference Table
| Action | When / How | Why It Helps |
|---|---|---|
| Close windows & doors | High‑pollen days (5‑10 am, late afternoon) | Prevents indoor pollen entry |
| Run AC on recirculate | Throughout the day | Filters indoor air |
| HEPA filter/purifier | Child’s bedroom | Captures pollen, dust‑mites, dander |
| Dehumidifier (<50 % RH) | Year‑round | Inhibits mold & dust‑mite growth |
| Wash bedding in hot water weekly | Weekly | Removes settled allergens |
| Dry laundry indoors | After each wash | Stops pollen from sticking to fabrics |
| Pet wipe‑down before entering home | Every outing | Reduces pet‑carried pollen |
| Wear hat, sunglasses, mask | Outdoor play on windy days | Blocks direct pollen contact |
| Nasal saline rinse | 2‑3× daily | Flushes inhaled pollen from nasal passages |
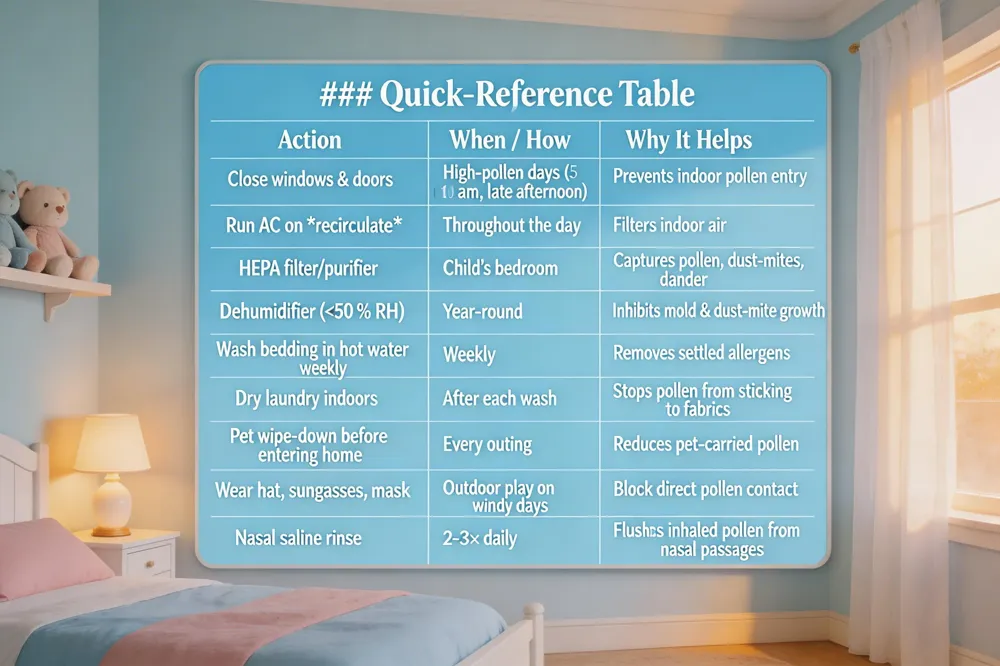 Keeping the indoor air clean is the first line of defense. Close windows and doors on high‑pollen days, run the air‑conditioner on recirculate mode, and install a HEPA‑rated filter or purifier in the child's bedroom. A dehumidifier set below 50 % humidity deters mold and dust‑mite growth, while allergen‑impermeable mattress and pillow covers further cut indoor allergen load.
Keeping the indoor air clean is the first line of defense. Close windows and doors on high‑pollen days, run the air‑conditioner on recirculate mode, and install a HEPA‑rated filter or purifier in the child's bedroom. A dehumidifier set below 50 % humidity deters mold and dust‑mite growth, while allergen‑impermeable mattress and pillow covers further cut indoor allergen load.
Outdoor activity timing matters: Pollen counts peak between 5 a.m. and 10 a.m. and again in the late afternoon. Check daily forecasts and plan play for mid‑day or after rain, and avoid lawn‑care chores that stir up pollen. When exposure is unavoidable, wear a wide‑brimmed hat and sunglasses, and consider a mask.
Laundry and pet management also limit pollen transfer. Dry clothes and bedding in a dryer instead of hanging them outside, and wash them weekly in hot water. Wipe pets with a damp towel before they enter the house and keep them out of the child's bedroom to reduce dander‑carried pollen.
For natural relief, encourage daily nasal saline rinses, keep the child well‑hydrated, and discuss any supplement use with a pediatrician. If symptoms persist despite these controls, consult a healthcare provider for antihistamines, nasal steroids, or referral to an allergist.
Medication Strategies for Spring Allergies
Medication Overview
| Class | Example(s) | Age | | Key Benefit | |-------|------------|----------|--------------| | Second‑generation antihistamines | Cetirizine, Loratadine, Fexofenadine | ≥ 2 yr | Relieves sneezing, itchy eyes, minimal drowsiness | | Nasal corticosteroids | Fluticasone, Budesonide, Triamcinolone | ≥ 4 yr (pediatric strength) | Reduces nasal inflammation, congestion | | Eye drops | Antihistamine/mast‑cell stabilizer, preservative‑free artificial tears | All ages (appropriate formulation) | Soothes watery, itchy eyes | | Oral hydrocortisone (low‑potency) | 1 % cream (topical) | All ages (topical) | Treats localized skin itching | | Immunotherapy | Subcutaneous shots, Sublingual tablets | 5‑yr + (often) | Long‑term desensitization | | Rescue epinephrine | Autoinjector (e.g., EpiPen) | Prescribed for anaphylaxis risk | Immediate reversal of severe reaction |
 When spring pollen spikes, the first line of defense is limiting exposure—keep windows closed, use HEPA‑filtered air‑conditioners, and shower promptly after outdoor play.
When spring pollen spikes, the first line of defense is limiting exposure—keep windows closed, use HEPA‑filtered air‑conditioners, and shower promptly after outdoor play.
Antihistamines – Second‑generation oral antihistamines such as cetirizine, loratadine, and fexofenadine are FDA‑approved for children 2 years and older. They relieve sneezing, itchy eyes, and post‑nasal drip without the drowsiness of first‑generation drugs.
Nasal corticosteroids – Daily intranasal steroids (fluticasone, budesonide, triamcinolone) are the most effective for persistent congestion and inflammation. Children as young as 4 years can use pediatric‑strength sprays; benefits appear after several days of consistent use.
Eye drops – Topical antihistamine or mast‑cell stabilizer drops, plus preservative‑free artificial tears, calm watery, itchy eyes. Avoid vasoconstrictor drops longer than 2‑3 days to prevent rebound redness.
Immunotherapy – For children whose symptoms remain uncontrolled despite environmental controls and OTC meds, referral to a pediatric allergist for skin‑prick testing and allergy immunotherapy (subcutaneous shots or sublingual tablets) offers long‑term desensitization.
Q&A
- How to get rid of springtime allergies? Limit exposure, wear masks on windy days, shower after outdoors, and use OTC antihistamines or nasal steroids; see a pediatrician if symptoms interfere with school or sports.
- Best kids allergy medicine for post‑nasal drip? Cetirizine or loratadine once daily plus a pediatric steroid nasal spray; add saline rinses for moisture.
- Best kids allergy medicine for itchy skin? Low‑potency hydrocortisone cream plus an oral antihistamine (cetirizine, loratadine, or fexofenadine).
- Best allergy medicine for a 5‑year‑old? Liquid cetirizine or loratadine; consider a Children’s Flonase nasal spray for congestion.
- Kids seasonal allergies medicine? Combine a daily oral antihistamine with a nasal steroid spray; add antihistamine eye drops if needed.
Always confirm dosing and formulation with your child’s pediatrician before starting any new medication.
Managing Skin Allergies and Rashes
Simple‑ Management Table
| Step | Action | Notes |
|---|---|---|
| 1️⃣ Clean | Lukewarm bath, gentle soap | Remove irritants |
| 2️⃣ Moisturize | Fragrance‑free, hypoallergenic cream | Apply while skin is damp |
| 3️⃣ Topical steroid | 1 % hydrocortisone cream (OTC) | Up to 7 days, avoid large‑area use |
| 4️⃣ Antihistamine (oral) | Cetirizine, loratadine, fexofenadine (appropriate dose) | Controls itch, especially night‑time |
| 5️⃣ Cool compress | 10‑15 min, 2‑3 × daily | Reduces swelling |
| 6️⃣ Seek care | Rapid spread, blisters, fever, breathing difficulty | Call 911, use epinephrine if anaphylaxis |
 Skin allergies in children most often appear as eczema (atopic dermatitis), contact dermatitis, or hives—red, itchy patches that may swell or become scaly. Common triggers include foods such as eggs, milk, peanuts, environmental irritants like nickel, latex, scented soaps, insect bites, and airborne allergens (pollen, pet dander).
Skin allergies in children most often appear as eczema (atopic dermatitis), contact dermatitis, or hives—red, itchy patches that may swell or become scaly. Common triggers include foods such as eggs, milk, peanuts, environmental irritants like nickel, latex, scented soaps, insect bites, and airborne allergens (pollen, pet dander).
Home treatment – For mild reactions, keep the area clean and apply a cool compress for 10‑15 minutes. After a lukewarm bath, use a fragrance‑free, hypoallergenic moisturizer to restore the skin barrier. Over‑the‑counter 1 % hydrocortisone cream can reduce redness and itching, while an age‑appropriate oral antihistamine (e.g., cetirizine) may help control more intense itch. Dress the child in soft cotton and avoid known triggers.
When to seek professional care – If the rash spreads rapidly, develops blisters, is accompanied by fever, difficulty breathing, lip or tongue swelling, or involves multiple body systems, call 911 and use a prescribed epinephrine auto‑injector if available. Persistent or severe eczema may require prescription‑strength steroids or referral to an allergist for testing and long‑term management.
Keeping a symptom diary, washing hands frequently, and maintaining a low‑humidity, HEPA‑filtered indoor environment can further reduce flare‑ups.
Special Considerations for Toddlers and Infants
Key Practices for Ages 0‑3
| Recommendation | Details |
|---|---|
| Window & AC management | Keep windows shut; run AC on recirculate during high‑pollen mornings (5‑10 am). |
| Post‑play routine | Bathe child, change clothes, wash hands to remove pollen. |
| Nasal saline spray | Gentle, pediatric‑safe spray 2‑3× daily. |
| Antihistamine | Liquid cetirizine or loratadine (approved ≥ 2 yr); dose per pediatrician. |
| Steroid nasal spray | Low‑dose pediatric spray if congestion persists; avoid sedating antihistamines. |
| Monitoring food reactions | Watch for itching, hives, swelling within 1 hr after eating new foods; have epinephrine auto‑injector if prescribed. |
| Pet exposure | Keep pets out of nursery; HEPA vacuums; hand wash after handling pets. |
| Environmental controls** |
 Seasonal allergies toddler treatment – Keep windows shut and run the AC on recirculate during high‑pollen mornings (5‑10 a.m.). After outdoor play, bathe the child and change clothes to wash off pollen. A gentle nasal saline spray several times a day clears allergens, and a pediatric‑approved, non‑sedating oral antihistamine (cetirizine or loratadine) can be given once daily. If congestion persists, a low‑dose steroid nasal spray may be prescribed, but avoid sedating diphenhydramine.
Seasonal allergies toddler treatment – Keep windows shut and run the AC on recirculate during high‑pollen mornings (5‑10 a.m.). After outdoor play, bathe the child and change clothes to wash off pollen. A gentle nasal saline spray several times a day clears allergens, and a pediatric‑approved, non‑sedating oral antihistamine (cetirizine or loratadine) can be given once daily. If congestion persists, a low‑dose steroid nasal spray may be prescribed, but avoid sedating diphenhydramine.
Signs of food allergies in babies – Reactions can appear within minutes to an hour after eating. Mild signs include a runny itchy nose, itchy mouth, isolated hives, or a single vomiting episode. Severe clues are swelling of lips/face/tongue, widespread hives, wheezing, stridor, persistent vomiting/diarrhea, pale or bluish skin, or limpness. Stop the food immediately and contact a pediatrician; call 911 for severe reactions.
Toddler allergies treatment – Use age‑appropriate antihistamine syrup (cetirizine or loratadine) and add saline or steroid nasal spray plus pediatric eye drops for itchy eyes. Maintain a low‑allergen environment by washing hands, face, and clothing after play, and keep windows closed. Have an epinephrine auto‑injector ready if prescribed.
Seasonal allergies in a 3‑year‑old – Typical symptoms are sneezing, clear runny or stuffy nose, itchy watery eyes, sore throat, and dark under‑eye circles. Management mirrors toddler care: limit exposure, daily saline rinses, and second‑generation antihistamine syrup; a pediatrician may add a low‑dose steroid nasal spray if needed.
How to treat allergies in a 1‑year‑old – True seasonal allergies are rare; confirm with a pediatrician. If diagnosed, a liquid cetirizine or loratadine can be used once daily, with a prescribed steroid nasal spray for persistent congestion and eye drops for itching. Environmental controls—closed windows, HEPA filtration, regular bedding washes—are essential.
How to prevent pet allergies in babies – Early exposure (especially dogs) may foster tolerance, but keep pets out of the nursery, use HEPA purifiers, vacuum with HEPA filters, and wash hands after handling pets. Discuss timing and strategy with a pediatrician.
Seasonal allergies in babies treatment – Minimize exposure (closed windows, HEPA filter), use sterile saline nasal drops, and if prescribed, a pediatric antihistamine drop. Avoid OTC oral antihistamines under age two unless directed by a doctor.
How to prevent food allergies in babies during pregnancy – No need to avoid common allergens. Focus on a balanced, nutrient‑dense diet with omega‑3s and vitamin D, and discuss any changes with an obstetrician.
How to prevent allergies in babies – Exclusive breastfeeding for 4‑6 months, early introduction of single‑ingredient solids (including common allergens) between 4‑6 months, smoke‑free environment, indoor humidity <50 %, allergen‑proof bedding, and regular pediatric check‑ups are key strategies.
Long‑Term Prevention and Professional Guidance
Prevention Checklist
| Habit | Implementation |
|---|---|
| Exclusive breastfeeding | First 4‑6 months |
| Early allergen introduction | Single‑ingredient solids (egg, dairy, peanut, etc.) 4‑6 months |
| Low indoor humidity | < 50 % RH with dehumidifier |
| HEPA‑filtered air & allergen‑proof bedding | Continuous |
| Regular pediatric check‑ups | Monitor growth, symptoms, medication safety |
| Allergy testing | Skin‑prick or blood test when symptoms persist |
| Immunotherapy | Subcutaneous shots or SLIT for proven triggers |
| Action plan for anaphylaxis | Epinephrine auto‑injector on hand, educate caregivers |
 Seasonal allergies in children—often triggered by tree, grass, or weed pollen—cause sneezing, itchy eyes, runny or stuffy noses, and may flare asthma. Parents can curb exposure by keeping windows shut, using air‑conditioning on recirculate mode, and wash hands, face, and clothing after outdoor play. Over‑the‑counter antihistamines, nasal steroids, and eye drops help, but a pediatrician should approve any medication regimen. Early‑life habits lower future allergy risk: exclusive breastfeeding for the first four to six months, introducing single‑ingredient solid foods (including allergenic items like egg, dairy, and peanuts) between four and six months, and maintaining low indoor humidity with dust‑mite‑proof bedding and HEPA filtration. When symptoms persist despite these controls, referral to a pediatric allergist for skin or blood testing is essential; immunotherapy (shots or sublingual tablets) offers long‑term desensitization. Guidelines recommend a stepwise approach—avoidance, second‑generation antihistamines, intranasal steroids, and, if needed, biologics—while ensuring an emergency action plan for anaphylaxis. Regular follow‑up with healthcare providers keeps treatment safe and effective.
Seasonal allergies in children—often triggered by tree, grass, or weed pollen—cause sneezing, itchy eyes, runny or stuffy noses, and may flare asthma. Parents can curb exposure by keeping windows shut, using air‑conditioning on recirculate mode, and wash hands, face, and clothing after outdoor play. Over‑the‑counter antihistamines, nasal steroids, and eye drops help, but a pediatrician should approve any medication regimen. Early‑life habits lower future allergy risk: exclusive breastfeeding for the first four to six months, introducing single‑ingredient solid foods (including allergenic items like egg, dairy, and peanuts) between four and six months, and maintaining low indoor humidity with dust‑mite‑proof bedding and HEPA filtration. When symptoms persist despite these controls, referral to a pediatric allergist for skin or blood testing is essential; immunotherapy (shots or sublingual tablets) offers long‑term desensitization. Guidelines recommend a stepwise approach—avoidance, second‑generation antihistamines, intranasal steroids, and, if needed, biologics—while ensuring an emergency action plan for anaphylaxis. Regular follow‑up with healthcare providers keeps treatment safe and effective.
Putting It All Together
Key takeaways: seasonal allergies are common, early symptoms include sneezing, itchy eyes, and allergic shiners; limit exposure by staying indoors during peak pollen, showering, and using HEPA filters. Next steps: monitor pollen forecasts, consult a pediatrician, and consider allergist referral for persistent symptoms to improve health.
